By Glenn Ellis
Why do some of us say they were allergic to an antibiotic if we really aren’t?
Because some of us have been incorrectly told by our parents that we had an allergic reaction to something as a child. Often, we had a side effect like a rash, nausea, diarrhea or headache. But a true allergic reaction is very different: Your body treats the medication as if it is an invader and releases chemicals to attack it. Contrary to popular belief, these reactions do not occur the first time you are exposed to a medication, because your body must be primed to recognize it. And some of us simply don’t like the idea of taking a medication and list it as an allergy so they will never be given it.
Whether you’re really allergic to penicillin, or just thinking you are, you could be at greater risk of superbug infections!
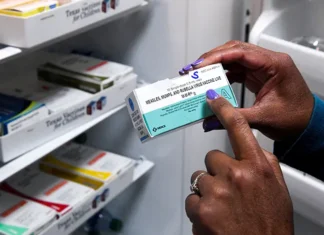
A new study has found patients who have penicillin allergies listed on their medical records are at an increased risk of developing superbug infections, largely because other antibiotics and alternatives could actually be fueling the development of bacteria that is drug resistant.
According to the report, penicillin is actually the most commonly documented drug allergy, noted by around 10 per cent of patients. Researchers set out to examine the relation between a penicillin allergy and the development of both MRSA and C difficile; both very nasty infections. People believed to have a penicillin allergy are often prescribed much stronger antibiotics that can raise their risk for dangerous infections.
The risk is largely due to the use of more broad spectrum antibiotics as alternatives to penicillin that may be fueling the development of drug resistant bacteria. Broad-spectrum antibiotics target a wide range of bacteria, but can increase the risk of antibiotic resistance and of dangerous infections by killing off beneficial bacteria in the gastrointestinal tract. These ‘broad-spectrum’ antibiotics allow bacteria to evolve into superbugs which can be deadly in the vulnerable and elderly.
Approximately one percent of people are colonized with the antibiotic-resistant form of staph aureus (known as MRSA). The percentage is higher for people who have been recently hospitalized.
C. Diff, on the other hand, lives all around us, too, including in human digestive systems. The problem with this superbug is that it won’t cause problems until the person begins to take antibiotics for another illness. At that point, the C. Diff can colonize out of control making the infected person much sicker.
Superbugs are invisible and can survive on surfaces for up to three days. That means that they can be transferred when one infected person simply touches another person.
Once an antibiotic is listed in your medical record as an allergy — even if you later admit it was never confirmed, or was really a minor side effect — nobody will want to give it to you. Doctors will be hesitant to prescribe it and pharmacists to dispense it, for fear that if something did go wrong, they would be held liable. In cases of superbug infections, this may leave you with no appropriate alternatives to cure your infection.
When you mistakenly (or on purpose) say you are allergic to a common antibiotic like penicillin, what would otherwise be a simple infections is more likely to be treated with antibiotics that target a broader range of bacteria. This leads to increased antibiotic resistance, creating even more superbug infections.
We do not have an endless choice of antibiotics to treat all infections. From MRSA to C. difficile diarrhea, superbug infections are becoming more common. And the more antibiotics you incorrectly list as drug allergies, the more infections you could potentially be left vulnerable to.
Suspected penicillin allergies can be easily confirmed with a skin test, but unfortunately there aren’t standardized allergy tests for other antibiotics. If patients are worried that they might be allergic to one of these antibiotics, the best step is to discuss the side effects they experienced with a doctor, and let him or her decide.
While children may show signs of being allergic to penicillin, this can often be a simple skin reaction caused by a virus. Even those with a positive diagnosis may no longer be allergic to penicillin a decade later, as their immune system ‘forgets’ its reaction to the drug.
The Takeaway? People believed to have a penicillin allergy are often prescribed much stronger antibiotics that can raise their risk for dangerous infections that may be untreatable. Testing folks to make sure they really are allergic to penicillin could lower that danger. We now know that more than 95 percent of patients with an indication of a penicillin allergy in their medical record are found not to be truly allergic, if tested by an allergist. Get tested if you’re not sure…
Remember, I’m not a doctor. I just sound like one.
Take good care of yourself and live the best life possible!
The information included in this column is for educational purposes only. It is not intended nor implied to be a substitute for professional medical advice. The reader should always consult his or her healthcare provider to determine the appropriateness of the information for their own situation or if they have any questions regarding a medical condition or treatment plan.
Glenn Ellis, is a Health Advocacy Communications Specialist. He is the author of Which Doctor?, and Information is the Best Medicine.